
AI in UK healthcare: Statistics, policies, and key challenges

Adopting AI in healthcare presents real challenges, including regulatory gaps and data security risks, as well as the need to train staff and integrate tools across hospitals, clinics, labs, and research centres. Organisations feel pressure to modernise, yet many still struggle to create conditions in which AI supports clinical teams rather than adding friction.
As an AI-first development partner deeply involved in healthcare innovation, Vention takes a closer look at the current state of AI in UK healthcare to assess how ready the system is for meaningful adoption. You’ll gain the latest insights on the topic and lay the groundwork for the operational peace of mind that comes from choosing the right approach early on.
About Vention
At Vention, decades of engineering experience meet a long-standing commitment to building healthcare technology. We’ve worked in the sector since our early days, and it remains one of our core industries. That experience shapes how we help UK organisations build secure, scalable digital products that meet regulatory requirements.
Today, Vention brings its deep, hands-on AI expertise to help healthcare providers move from experimentation to real-world impact. From telehealth applications and medical imaging systems to EHR platforms and digital pharmacy solutions, we develop bespoke healthcare solutions powered by advanced AI capabilities, which gives organisations confidence in every line of code.
Years in healthcare software development
Healthtech projects delivered
In funding raised by our healthcare clients
Helping deliver software systems compliant with UK regulations
ISO 27001-certified to ensure the safety of our clients’ data
Internal AI Centre of Excellence providing the latest insights and innovations to strengthen every healthcare project

A general overview of the AI market size in the UK
The United Kingdom ranks third globally for AI market valuation, following the United States and China. The valuation of the UK AI sector is estimated at £17.2 billion in 2025. The UK AI sector is larger than those of all other European countries.
AI adoption rate in the UK across all industries, %
Q3’23
Q4’23
Q1’24
Q2’24
Q3’24
Q4’24
Q1’25
Q2’25
Q3’25
Q4’25
The number of AI companies has risen sharply from 3,713 in 2023 to 5,862 in 2024, an increase of 58%. The revenue has grown too: up 68% to £23.9 billion in 2024.
Sources: [1], [2], [3], [54]
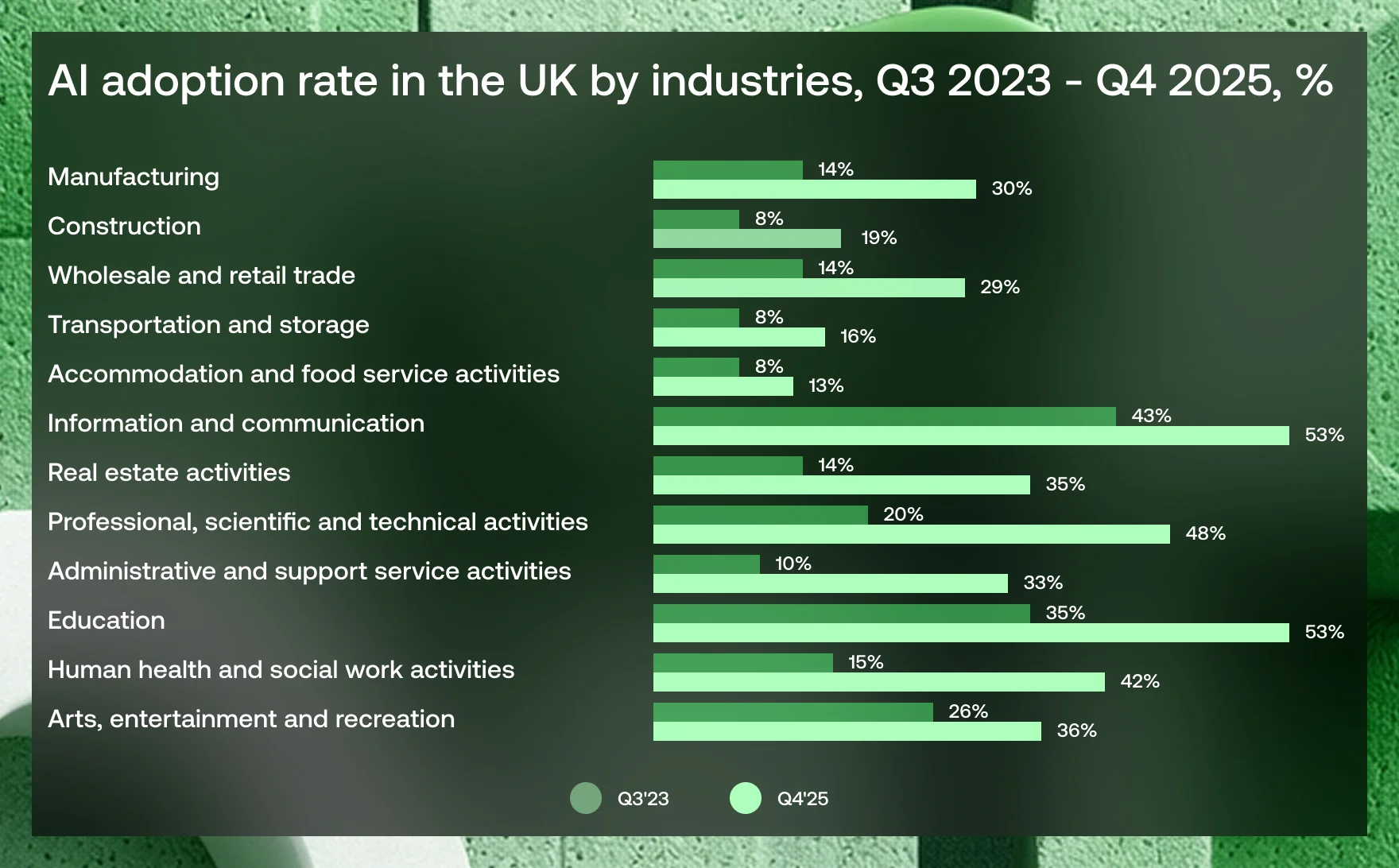
AI uptake across sectors in the UK
In 2025, the UK healthcare industry not only recorded one of the highest adoption rates at 42%, but also posted one of the strongest growth rates between 2023 and 2025, at 27%.
A deep dive into AI in UK healthcare
The valuation of the UK AI healthcare market reached ~£312.94 million in 2025. Forecasts indicate that the UK market of AI in healthcare will reach ~£2.23 billion by 2034. The projected compound annual growth rate of the AI healthcare market in the UK is 24.35%.
Fundraising for AI companies in the UK healthcare
In 2025, UK AI startups raised ~£5.84 billion, up 80% compared to 2024 and accounting for 33% of all UK venture capital raised this year. Leading areas of UK health AI investment in 2025 include AI drug discovery, metabolic health, neurology, and synthetic biology.
Sources: [4], [5]
London leads UK AI fundraising in healthcare and life sciences sectors
As the country’s business hub, London attracts the highest concentration of healthcare AI investment. In 2024, health AI startups based in the capital raised £411 million, nearly half of the UK total. Companies like Flo Health, Huma, Basecamp Research, LabGenius, Relation Therapeutics, Scarlet, IMU Biosciences, Bioniq, Limbic AI, and Baseimmune raised funding exceeding £7 million each.
In 2025, London’s life sciences and biotech companies attracted approximately £1.55 billion in investment, making the UK capital the top city outside the US in this sector.
Sources: [6], [55]
Who regulates AI in UK healthcare?
AI in healthcare spans several regulatory domains in the United Kingdom, which means multiple bodies are directly involved in oversight.
Sources: [7], [8], [9], [59]
MHRA (Medicines and Healthcare products Regulatory Agency)
The primary regulator for medical devices, including software as a medical device, and now, AI as a medical device (AIaMD).
To facilitate innovative initiatives, including AI-powered ones, MHRA has waived fees from January 2026 for micro and small UK firms in a pilot scheme to help facilitate high-potential ideas that might otherwise stall due to early costs.
NICE (National Institute for Health and Care Excellence)
NICE evaluates, guides, and oversees the adoption of AI tools in clinical practice. In 2022, NICE updated its evidence standards framework for digital health technologies to include requirements for AI and data-driven systems with adaptive algorithms.
CQC (Care Quality Commission)
CQC steps in when AI systems become a part of regulated care services. While the CQC is still shaping its approach to AI, it has already issued guidance (GP Mythbuster 109: Use of artificial intelligence (AI) in GP services) outlining what inspectors will review when GP practices deploy AI.
Government initiatives and policies for AI in healthcare in the UK
The United Kingdom is taking an active role in shaping the safe, responsible, and sustainable adoption of AI in healthcare. UK regulators are developing guidance, updating standards, and refining oversight to manage the rapid growth of AI-enabled technologies in clinical and operational settings.
AI and Digital Regulations Service for health and social care
Regulators in the United Kingdom each maintain their own frameworks and guidance, which can make it difficult for organisations to navigate the requirements for AI in health and social care.
To simplify the process, the UK government created the AI and Digital Regulations Service. The service was commissioned by NHS England and developed in collaboration with NICE, MHRA, HRA, and CQC. The AI and Digital Regulations Service serves as a central pathway, which outlines the requirements for AI technology developers and adopters, highlights relevant standards, and provides regular regulatory updates.
Source: [10]
Software and AI as a Medical Device Change Programme
Launched by the MHRA, the programme sets out clear regulatory requirements for the development of software and AI tools for healthcare, with patient safety at its core. It addresses the unique challenges of creating and implementing SaMD and AI as Medical Devices, while ensuring that the UK is recognised globally as a home for innovation in this field.
Source: [11]
NHS AI Lab
Launched in 2019, the NHS AI Lab plays a central role in advancing the safe and effective use of AI across healthcare. It oversees the development, testing, and deployment of AI solutions within the NHS, driving innovation while shaping long-term strategy and standards. Through its work, the government has gained clearer insight into the realities of large-scale AI adoption, including technical constraints, regulatory hurdles, and workforce readiness.
Sources: [12], [13]
AI Airlock
Traditional medical device and software regulations were not designed with AI in mind. To address this, the MHRA and the NHS AI Lab launched the AI Airlock in 2024, a regulatory sandbox for AI as a Medical Device (AIaMD) products. The Airlock enables companies to collaborate directly with regulators, trial AI health solutions in a supervised, safe-to-fail environment, and clarify compliance pathways.
The first pilot phase ran until April 2025 and included four projects:
- Radiology report generation (Philips)
- AI performance monitoring (Newton’s Tree Federated AI Monitoring Service)
- Oncology pathway support (OncoFlow)
- RAG-based clinical guidance agent (Automedica)
The pilot proved successful enough to warrant a second phase for 2025-2026. Its findings are already influencing regulatory thinking at the MHRA and across UK bodies, shaping future rules, guidance, and oversight mechanisms for AIaMD.
Source: [14]
HealthAI Global Regulatory Network
In June 2025, the United Kingdom became the first country to join the HealthAI Global Regulatory Network, an international coalition of health regulators committed to the safe and effective use of AI in healthcare. Membership strengthens the MHRA’s role in shaping global standards and advancing responsible AI adoption across health and care systems.
Source: [15]
AI in Health and Care Awards
The AI in Health and Care Awards programme accelerates the testing and deployment of AI technologies across the NHS. Established in 2019, it supports the development of AI tools that help manage health conditions, improve the speed and accuracy of diagnosis, tackle COVID backlogs, and reduce waiting lists.
In the third round of the AI in Health and Care Awards, nine companies received a total investment of £16 million to trial and scale AI solutions aimed at:
- Running faster and more accurate cancer checks
- Diagnosing rare diseases
- Identifying women at the highest risk of premature birth.
Sources: [16], [17]
AI adoption among UK clinics and hospitals: Taking the lead or falling behind?
Government support for AI in healthcare is strong in the United Kingdom, yet adoption across clinics and hospitals remains uneven. Many NHS organisations recognise the value of AI, but real-world deployment across clinical pathways continues to progress slowly.
Adoption levels vary across professional groups, yet most categories expect to integrate AI tools into their work in the near future.
of NHS staff support the use of AI for patient care
of NHS staff back AI usage in administrative processes
of healthcare staff report that they are keen to use AI in their daily work
of the NHS staff think AI will make them feel more distant from patients

NHS staff response rate when asked to what extent they agree with the statement 'I look forward to using AI as part of my job'?
Don’t know
Disagree
Neither agree nor disagree
Agree
Source: [18]

The current level of AI adoption among NHS organisations in the UK, 2025
Advanced adoption
Don’t know
No adoption
Moderate adoption
Early stages
The main factors influencing decisions to adopt AI technologies in healthcare organisations
Don't know
Health equity
Patient/carer demand
Industry push
Internal leadership
Political pressure
Tech advancement
Clear problem need
Staff efficiency
Patient outcome
Cost saving
Source: [22]
How GPs across the UK are using AI
The UK is still on the way to a consistent national guidance on AI. Yet, despite the lack of formal AI training and the intense pressure general practitioners face today, many have begun adopting AI, either independently or as part of their practice.
- 28% of GPs in the UK use AI in their practice
- 13% of all GPs use tools provided by their practice
- 11% use tools they have obtained independently
- 31% of GPs in England and 20% of GPs in Wales use AI compared to just 20% and 9% in Scotland and Northern Ireland, respectively
Source: [57]
AI tools used by GPs for administrative and supportive tasks
AI usage
AI tools and tasks performed
Clinical documentation and note-taking
57%
- Heidi Health, AccurX Scribe, and Lexacom are ambient voice technologies (AVTs) that capture and process clinical conversations to help GPs generate consultation summaries, translate patient interactions, and draft referral letters
Professional development/CPD
45%
- ChatGPT for capturing trainees’ portfolio activities and enabling reflection on their clinical experiences
- ChatGPT study mode is a study setting that provides step-by-step guidance rather than quick answers, which enables users to work through clinical cases, test their knowledge, and prepare for assessments
- Glass Health for learning through practising with simulated clinical cases.
Administrative tasks
44%
- Heidi Health, AccurX Scribe, Lexacom for drafting referral letters and communications
- ChatGPT, Claude, and Copilot for drafting referral letters and communications, and capturing practice meeting notes
- Ankit AI for creating policies and governance documents
- Patchs for digital triage that involves analysing patient requests before appointments to prioritise patient cases based on clinical need
Clinical decision-making
28%
- ChatGPT and Claude for answering clinical questions
- Glass Health for generating management plans, differential diagnoses, and answering clinical questions
- Mediwise for flagging important guidelines
- C the Signs for early cancer detection
- Anima for managing patient requests and total triage
Source: [57]
A real-life NHS case of AI adoption: Progress slowed by practical realities
By 2023, the government had already invested £123 million in 86 AI technologies through the AI in Health and Care Awards. In the same year, the NHS also launched a programme to accelerate AI adoption for diagnosing chest conditions, including lung cancer, across 66 NHS trusts.
While the initiative sounded promising, implementation has been more complex. Contracting processes took four to ten months longer than anticipated, and by June 2025, a third of the participating trusts had yet to deploy the technology in clinical practice.
Sources: [19], [20], [21]
Use cases and benefits of AI in healthcare
The potential applications of AI in healthcare in the United Kingdom are extensive. AI technologies can support clinicians with faster diagnoses, streamline administrative workflows, and enable more personalised treatment pathways across a broad range of clinical and operational tasks.
Many AI tools in healthcare have not yet been tested at scale in real-world NHS environments. The limited scale of real-world testing makes it difficult to draw firm conclusions about long-term effectiveness. Organisations will need time, structured evaluation, and sufficient resources to validate impact and demonstrate measurable value as deployment increases.
Sources: [22], [23]
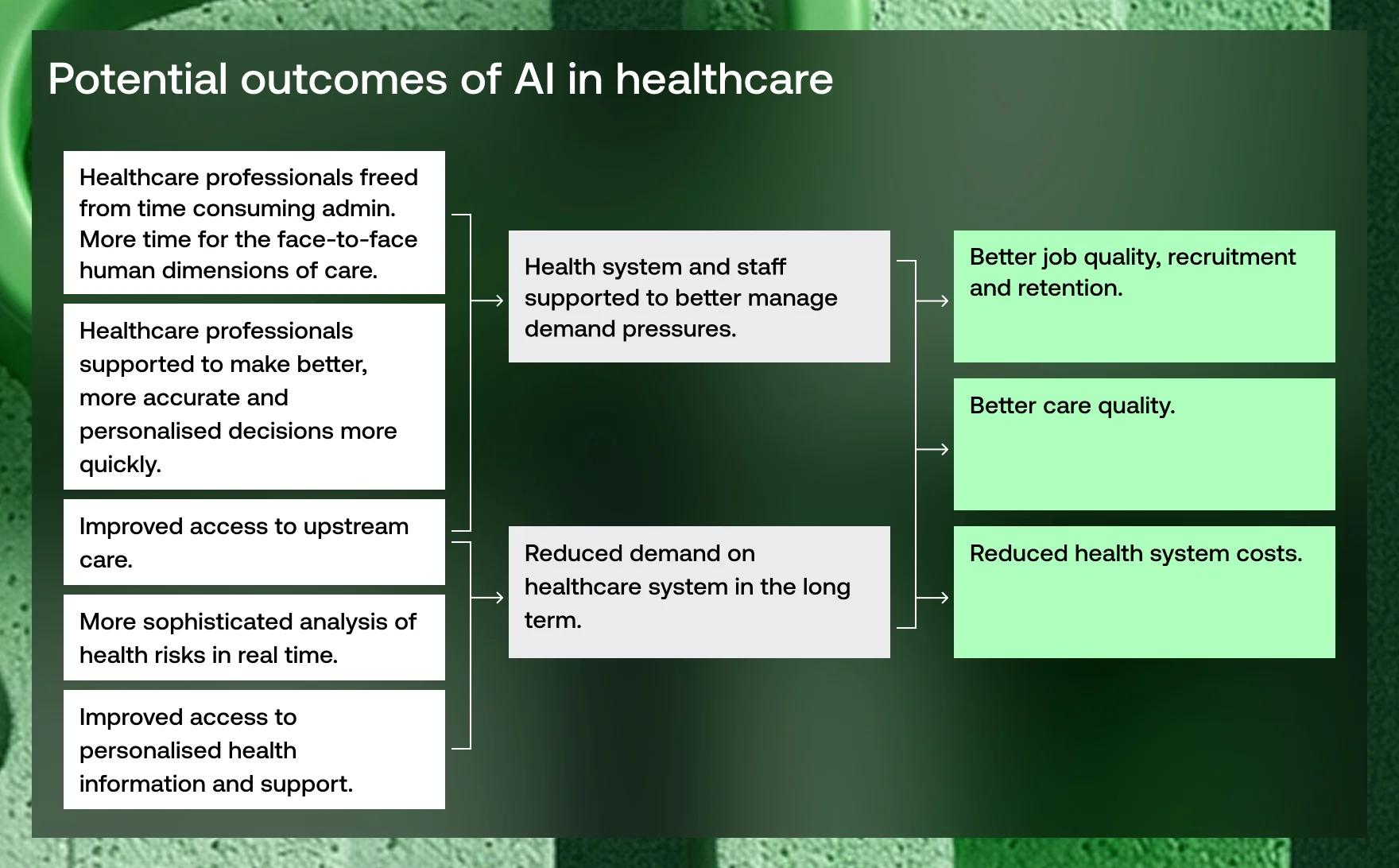
AI for healthcare organisation and administrative activities
On average, clinicians dedicate 13.5 hours per week (and 16.5 hours per week for consultant nurses) to creating, updating, and managing patient records. Between three and five hours of administrative work per week is often completed in clinicians’ personal time.
Historically, technologies and tools for administrative purposes have received less attention from policymakers. Yet, such technologies tend to carry less clinical risk, which makes them an attractive opportunity to explore the possibilities of AI:
- 31% of the public and 32% of NHS staff cite reducing administrative burdens for healthcare staff as the top benefit of AI.
- 22% of London-based clinics that already adopted AI report improved administrative efficiency, and 21% highlight increased availability of staff time for patient-facing work.
Sources: [18], [22], [24]
NHS AI trial to support administrative workflows
Microsoft 365 Copilot, deployed as a pilot project across 90 NHS organisations and more than 30,000 NHS workers, has proved to deliver unprecedented value.
The results show that AI-powered administrative support could save NHS staff, on average, 43 minutes per staff member per day. That’s 400,000 hours of staff time per month that could be effectively spent on delivering frontline care.
Source: 58

AI adoption for clinical decision-making in the UK
Research published in 2024 by The Alan Turing Institute found that 16% of doctors using AI in their work relied on diagnostic and decision-support systems powered by AI. The most common applications were image processing, risk assessment, and triage.

Common application areas of AI diagnostic and decision support systems, %
Electrocardiogram (ECG) or cardiotocography (CTG)
Prognosis or diagnosis
Risk assessment and triage
Image processing
In London, where AI adoption is advancing more quickly, 10% of clinics using AI reported improvements in decision-making, and 6% highlighted better clinical outcomes.
Sources: [22], [25]

AI for healthcare service delivery
AI-powered applications, chatbots, wearables, and smart devices can help patients access therapies, receive health information, follow prescribed treatments, and manage ongoing conditions more effectively.

Using AI in triage and navigation services within general practice (GP) could free up 29 million GP appointments per year. For NHS 111 and GP call handlers and receptionists alone, this could translate into immediate productivity gains valued at £340 million annually.
Another example highlights the main benefits of AI-based mental health chatbots that people choose:
- 50% of respondents note that they value the high-speed support they receive.
- 46% mention better accessibility to mental health assistance.
Sources: [26], [27]
The use of AI for population health data analysis
AI can be applied to analyse large-scale, population-level datasets and generate novel, real-time insights that inform public health strategies.
For example:
- Tracking epidemics or patterns of disease spread, e.g., as it was during the COVID-19 pandemic
- Identifying individuals or groups at higher risk of developing particular conditions to ensure earlier intervention.

AI in drug discovery
The UK is home to 79 companies that stand at the forefront of AI adoption in the pharmaceutical sector, ranking first in Europe and fourth globally, behind only the United States, China, and South Korea.

In February 2025, the government announced £82.6 million in funding for three major research projects. Two of these projects will leverage AI to develop new treatments and diagnostics for diseases such as cancer and Alzheimer’s.
To further cement the UK’s position as a hub for AI-driven drug discovery, the OpenBind consortium is building the world’s largest dataset (20 times larger than anything gathered in the past 50 years), mapping how drugs interact with proteins in the human body. Estimates suggest that AI could reduce the cost of drug discovery and development by up to £100 billion.
Sources: [28], [29], [30]

Planning your next step in AI healthtech?
We'll help you successfully navigate development, compliance, data, and scaling.
Real-life success stories of AI in the UK healthcare
AI for hospital discharge summary generation
Through its Federated Data Platform, the NHS has introduced a tool that assists clinicians in drafting discharge summary letters using information from patients’ medical records at a given trust. The AI-generated draft is then reviewed and finalised by the responsible clinician before being shared with the patient and their GP.
The tool reduces administrative workload and gives NHS staff more time to focus on high-quality care.
Source: [31]
NHS AI for better patient care
More than 360,000 patients attend A&E on five or more occasions each year, often due to loneliness, mental health conditions, or chronic illness. The volume of repeat attendance places significant pressure on emergency services.
To address the issue, the NHS is now using AI to identify patients most at risk of becoming frequent attenders. Instead of waiting for another emergency visit, the NHS proactively reaches out with tailored support. Early results indicate that this approach can reduce repeat A&E visits by over 50%, improving patient wellbeing while relieving pressure on hospitals.
Source: [53]
AI scripting pilot by NHS
Oxford University Hospitals NHS Foundation Trust launched a pilot of an ambient voice technology that captures conversations between patients and clients during appointments and generates transcriptions and clinical summaries using AI. As of 2026, eight in 10 technology users have already reported reduced time spent on documentation, which allows doctors to save from one to ten minutes and focus more on patients.
Source: [56]
Melo by Decently
Digital health startup Decently has developed Melo, an AI-powered tool designed to help clinicians manage, support, and improve the lives of patients with brain injuries and neurological complexities such as dementia or autism.
Already in use across several UK hospitals, Melo enables healthcare professionals to:
- Complete, track, and review assessments digitally, reducing the time required to complete an individual patient assessment by 89%.
- Build personal profiles to support more holistic and person-centred care.
- Automatically visualise trends and changes in patient behaviour, with eight in ten users confirming improved patient behaviour analysis.
- Get AI-generated insights and summaries for better clinical decisions.
Source: [32]
C the Signs
C the Signs is a clinical decision-support tool that helps GPs detect cancer earlier by analysing combinations of symptoms, risk factors, and clinical data. The system integrates with major GP record platforms such as EMIS and SystmOne, and provides prompts to clinicians in under 30 seconds.
The tool has already shown a measurable impact: in practices using C the Signs, cancer detection rates rose from 58.7% to 66%, reflecting a significant improvement of 12.3 percentage points.
Sources: [33], [38]
BenevolentAI
BenevolentAI is a UK-based company that applies artificial intelligence to speed up and improve drug discovery. Its AI models help scientists identify new disease targets, predict how potential drugs might work, and set up experiments more effectively.
Since 2019, AstraZeneca has partnered with BenevolentAI to use these tools to identify novel drug targets, particularly in conditions such as chronic kidney disease and idiopathic pulmonary fibrosis.
Source: [34]
POPDx
Using data from the UK Biobank, researchers at Stanford developed a machine learning framework called POPDx that predicts a wide range of diseases, including rare ones. By combining patient data with knowledge about disease relationships, the system identifies hidden health risks more quickly and accurately.
The breakthrough demonstrates how machine learning can accelerate diagnosis and give clinicians more time to focus on the patients who need it most.
Sources: [39], [40]
Talk It Out: AI chat therapy
Part of the UK’s startup incubation ecosystem at the STFC Business Incubation Centre, Talk It Out is a digital wellbeing app that offers an AI conversational companion, Ori, to support users with day-to-day emotional health. Users can journal or speak freely, and Ori responds naturally to help them explore their feelings and gain personal insight.
The app is built around privacy, non-judgmental listening, and 24/7 availability, making mental health support more accessible.
Source: [35]
Leaf AI
Operating under the brand Lola Cares, Leaf AI applies conversational and assistive AI in adult social care settings. The company developed a platform to support people with social isolation and loneliness, as well as individuals with dementia, autism, and acquired brain injury, by offering tools for memory, personal connection, and companionship.
In addition to improving the quality of life for service users, Leaf AI also reduces the administrative burden on care providers. By simplifying statutory reporting to the Care Quality Commission (CQC), the platform can save up to 80% of admin time.
Sources: [36], [37]
The attitude of the UK public towards healthcare AI tools
Awareness of AI in healthcare remains mixed. Around 46% of UK adults have heard about AI being used in healthcare, while 44% say they have not come across its use in the sector.
Overall, public sentiment supports AI adoption within the NHS. Confidence in full automation, however, remains low. Only 9% of the UK public believe that AI will eventually replace doctors.
The level of UK public approval of AI adoption in the UK healthcare
Supportive
Not supportive
For patient care
54%
33%
For administrative purposes
61%
28%

The strongest areas of support are in medical imaging:

- 61% back the use of AI to speed up CT and MRI processes.
- 59% support AI analysing scans in real time alongside radiologists.
- 54% agree to AI assistance in identifying problems on medical images.
The main reasons for public distrust towards AI in healthcare include a perceived lack of empathy and concerns about incorrect decisions made by AI.
- 24% of UK adults believe AI systems cannot display empathy or kindness.
- 53% fear they will feel more distant from healthcare professionals.
Sources: [18], [51]
How age shapes attitudes towards AI in healthcare
Younger people, aged 16-24, are most sceptical about the benefits of AI for care quality, whilst the UK public aged 25-34 is most sure of AI's usefulness for care quality.
The percentage of people who think that using AI will make the quality of health care better, and their age group
16-24
25-34
35-44
45-54
55-64
65+
Source: [18]
Will AI change the quality of healthcare services?
When it comes to expectations, 31% of people in the UK believe that greater use of AI will improve public health in the next three to five years. By contrast, 43% expect no real change, even with wider adoption.
Another study suggests that perceptions of AI’s broader impact on care quality are divided.
Sources: [18], [42]
Challenges on the road to AI-driven healthcare in the UK
Although the potential of AI in healthcare is significant, adoption still faces several structural, organisational, and public-facing barriers.
Organisational readiness and digital maturity
Successfully integrating AI requires a strong digital foundation. Although 86% of NHS organisations now have some form of electronic patient record, only 20% can be considered digitally mature. In social care, the gap is even wider: just 45% of providers use digital care records, which limits their ability to adopt AI across health and care services.
Basic infrastructure remains a barrier. 35% of NSH trust leaders cite poor wi-fi, outdated computers, and other technology issues as obstacles to digital progress. As a result, around 90% of AI tools remain stuck in pilot phases. Most fail to scale beyond a single trust due to limited digital infrastructure and the absence of permanent IT systems that support deployment across multiple trusts.
Sources: [42], [43], [52]
Public trust, privacy, and security concerns
The NHS is highly trusted for data sharing (by 85% of the UK public), but security concerns remain a leading barrier to the broader adoption of AI in healthcare. The top concern, cited by 57% of UK adults, is that their data may not be stored securely or could be hacked or stolen.
Oversight is another concern. 30% of the public believes healthcare professionals may not challenge AI-generated decisions, which adds to uncertainty around the tools’ reliability.
Sources: [18], [44]
Funding constraints
73% of NHS trust leaders cite funding as the number one barrier to digital transformation, including AI adoption.
In 2024, the Department of Health and Social Care slashed the NHS AI Lab’s budget from the originally promised £250 million to £139 million, complicating plans to scale AI initiatives.
Commenting on the cut, Pritesh Mistry, policy fellow for digital technologies at the King’s Fund, told Digital Health News: “A cut in funding is obviously going to have implications for the progress of implementation of AI into the NHS, and one of the challenges with deploying technology into the NHS is that there is a lot of short-term funding.”
Source: [45]
Bias, equity, and representative data
A 2024 equity review of medical devices identified unfair bias risks across multiple technologies, including AI-enabled tools. These risks disproportionately affect minority ethnic groups and raise concerns about unequal outcomes.
The government has since called for coordinated action to reduce these risks. The priority is to ensure that data used throughout the lifecycle of AI-enabled medical devices is more representative, from early concept and design through development and testing to NHS deployment.
Source: [46]
Healthcare staff readiness
In a recent report by the AHSN Network AI Initiative Core Advisory Group, 87% of respondents agreed that building staff capacity and capability (read ‘staff training’) is vital to realising AI’s potential.
However, despite this interest and the availability of some training, many health and care professionals face barriers linked to workload and time pressures. According to the 2024 NHS Staff Survey, only 34% of staff felt they had enough colleagues to do their job properly, and fewer than half (47%) reported being able to meet all the conflicting demands on their time.
Sources: [18], [47], [48]
When it comes to the use of AI, transparency is essential
Most people want to be informed when AI is used in their care. 69% of adults aged 16-64 and 82% of adults aged 65+ say they should be told when AI is involved in diagnosing illness. Even for administrative tasks such as generating appointment letters, 55% believe disclosure is necessary.
Source: [18]
GPs' concerns on large-scale AI adoption
Most people want to be informed when AI is used in their care. 69% of adults aged 16-64 and 82% of adults aged 65+ say they should be told when AI is involved in diagnosing illness. Even for administrative tasks such as generating appointment letters, 55% believe disclosure is necessary.
Source: [18]
of AI non-users and 80% among those who use practice-selected AI tools mentioned professional liability and medico-legal issues
of AI non-users and 78% among those who use practice-selected AI tools cited a lack of regulatory oversight
among non-users and 69% among those who use practice-selected AI tools fear risks of clinical errors
among non-users and 69% among those who use practice-selected AI tools mention patient privacy and data security concerns
The future of AI in the UK economy, including health and care
AI is not expected to trigger widespread job losses in the UK healthcare sector, but it is likely to reshape roles and change how work is carried out.
Source: [18]
Where GPs see AI in the next years
For the next two to three years, GPs across the UK want artificial intelligence to help them more with admin tasks rather than involve AI in high-risk clinical decisions.
- 54% want AI to automate their administrative workflows
- 50% want AI to automate clinical documentation and note generation
- 31% want AI to enable patient education and provide self-care guidance
Source: [57]
How government policy is enabling AI at scale
At a national level, the government is taking steps to ensure the secure and sustainable adoption of AI across all sectors. In January 2025, the government published the AI Opportunities Action Plan, which outlines 50 recommendations designed to support AI adoption across the economy and public services. The recommendations span health, infrastructure, procurement, regulation, data, skills, and governance.
In the same month, the government confirmed its intention to implement all 50 recommendations. The announcement signals a strong commitment to embedding AI across both public and private spheres.
By 2027, NHS England plans to introduce the AI Research Screening Platform (AIR-SP), a centralised, secure cloud environment that will allow multiple AI tools to be tested across NHS trusts simultaneously. Backed by £6 million in government funding, the programme is expected to save from £2 to £3 million per multi-site study and significantly accelerate the rollout of AI solutions.
Sources: [1], [49], [50], [52]

Become the one who shapes the future of AI in health and care
Visit our London office or connect online. We’re eager to bring your innovative ideas to life.
Churchill Place
London E14 5RE, UK
List of sources
Sources
- AI Opportunities Action Plan, GOV.UK
- Grand View Research
- Artificial Intelligence sector study 2024, GOV.UK
- UK AI in Healthcare Market Report, IMARC Group
- UK Innovation Update Q2 2025, Dealroom
- London & Partners, London Hits All-Time High for Venture Capital Investment into AI in 2024
- Press release 30 April 2024, GOV.UK
- Policy paper: Implementing the UK’s AI regulatory principles: initial guidance for regulators, GOV.UK
- GP mythbuster 109: Use of artificial intelligence (AI) in GP services, CQC
- Understanding regulations of AI and digital technology in health and social care, NHS
- Guidance: Software and AI as a Medical Device Change Programme roadmap. GOV.UK
- Press release, Arden&GEM
- AI knowledge repository, NHS
- AI Airlock: the regulatory sandbox for AIaMD, GOV.UK
- HealthAI
- Press release 3 March 2023, GOV.UK
- Press release 24 June 2025, GOV.UK
- Analysis: AI in health care: what do the public and NHS staff think, The Health Foundation
- UCL News, 11 September 2025
- Press release 23 June 2023, GOV.UK
- Procurement and early deployment of artificial intelligence tools for chest diagnostics in NHS services in England: a rapid, mixed method evaluation
- AI in London healthcare: The reality behind the hype
- Principles for Artificial Intelligence (AI) and its application in healthcare, BMA
- Report: Assessing the burden of clinical documentation, Nuance
- Exploring doctors’ perspectives on AI after the emergence of large language models, The Alan Turing Institute
- Paper: Preparing the NHS for the AI Era: Why Smarter Triage and Navigation Mean Better Health Care
- How do people feel about AI, The Alan Turing Institute
- Press release 11 February 2025, GOV.UK
- From Code to Cure: How AI is reshaping drug discovery, the UK's standing and the role of real estate, Knight Frank
- Press release 10 June 2025, The Nuffield Department of Medicine
- Artificial Intelligence Assisted Discharge Summary (AI Assisted DSUM) FDP product privacy notice, NHS England
- Melo
- C the Signs
- BenevolentAI
- Talk it Out
- Leaf AI
- UK Tech Investment News, 30 May 2024
- ASCO Publications, Journal of Clinical Oncology
- Press release 2 February 2023, Using Machine Learning to Predict Rare Diseases, Stanford University
- UK Biobank
- THE IPSOS AI MONITOR 2025
- Transformation Directorate: Our strategy to digitise, connect and transform, NHS England
- Press release 15 October 2024, NHS Providers
- Public attitudes to data and AI, Department for Science, Innovation and Technology
- Press release 3 June 2024, Digital Health
- Equity in medical devices: independent review, GOV.UK
- Accelerating Artificial Intelligence in health and care: results from a state of the nation survey
- NHS Staff Survey 2024
- Press release 14 January 2025, Digital Health
- AI Opportunities Action Plan: government response
- The Future of AI in Healthcare: Public perceptions of AI in Radiology
- Press release 22 September 2025, GOV.UK
- Press release 12 December 2024, NHS England
- UK’s Office for National Statistics Business Insights and Conditions Survey (Datasets)
- London & Partners, London Surges Ahead as Europe’s Life Sciences Capital
- Digital Health
- Nuffield Trust and Royal College of General Practitioners, How are GPs using AI, Research Report
- Press release 21 October 2025, GOV.UK
- Guidance, Clinical investigations for medical devices, GOV.UK




